Diabetes mellitus (DM) is classified on the basis of the pathogenic process that leads to hyperglycemia, as opposed to earlier criteria such as age of onset or type of therapy.
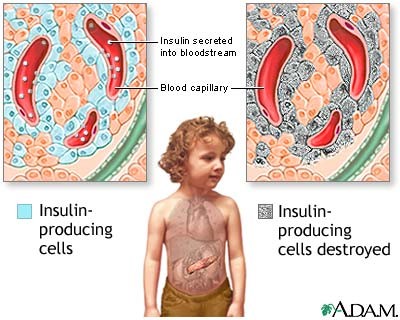
The two categories of DM are named as type I and type II. Type l is divided into I.A and I.B. DM results from autoimmune beta cell destruction, which leads to insulin deficiency.
Individuals with type l.B DM lack immunologic markers indicative of an autoimmune destructive process of the beta cells. However, they develop insulin deficiency by unknown mechanisms and are susceptible more to ketosis.
Relatively few patients with type I DM are in the type l.B. Many of them are either African- American or Asian in heritage.
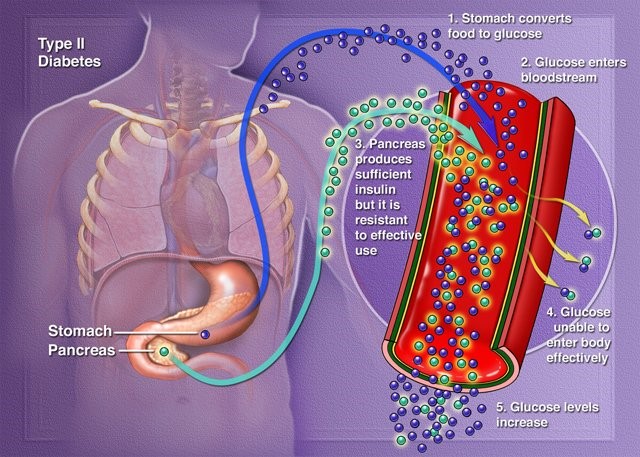
Type II DM is a heterogeneous group of disorders characterized by variable degrees of insulin resistance, impaired insulin secretion and increased glucose production.
Certain genetic and metabolic defects prognosis and follow-up for the 5-year survival rate after surgery is usually >95%, the recurrence rate is <1 0%.
After successful surgery, catecholamine excretion returns to normal range in about 2 weeks and should be measured to ensure 100% tumor removal. Catecholamine excretion should be assessed at the reappearance of suggestive symptoms or yearly in asymptomatic patients.
For malignant pheochromocytoma, the 5-year survival rate is usually <50%, although long-term survival is occasionally noted. Complete removal cures the hypertension in approximately three fourths of patients. In the remainder, hypertension recurs but is usually well controlled by standard antihypertensive agents.
In this group, either underlying essential hypertension or irreversible vascular damage induced by catecholamines may cause the persistence of the hypertension.